Definition:
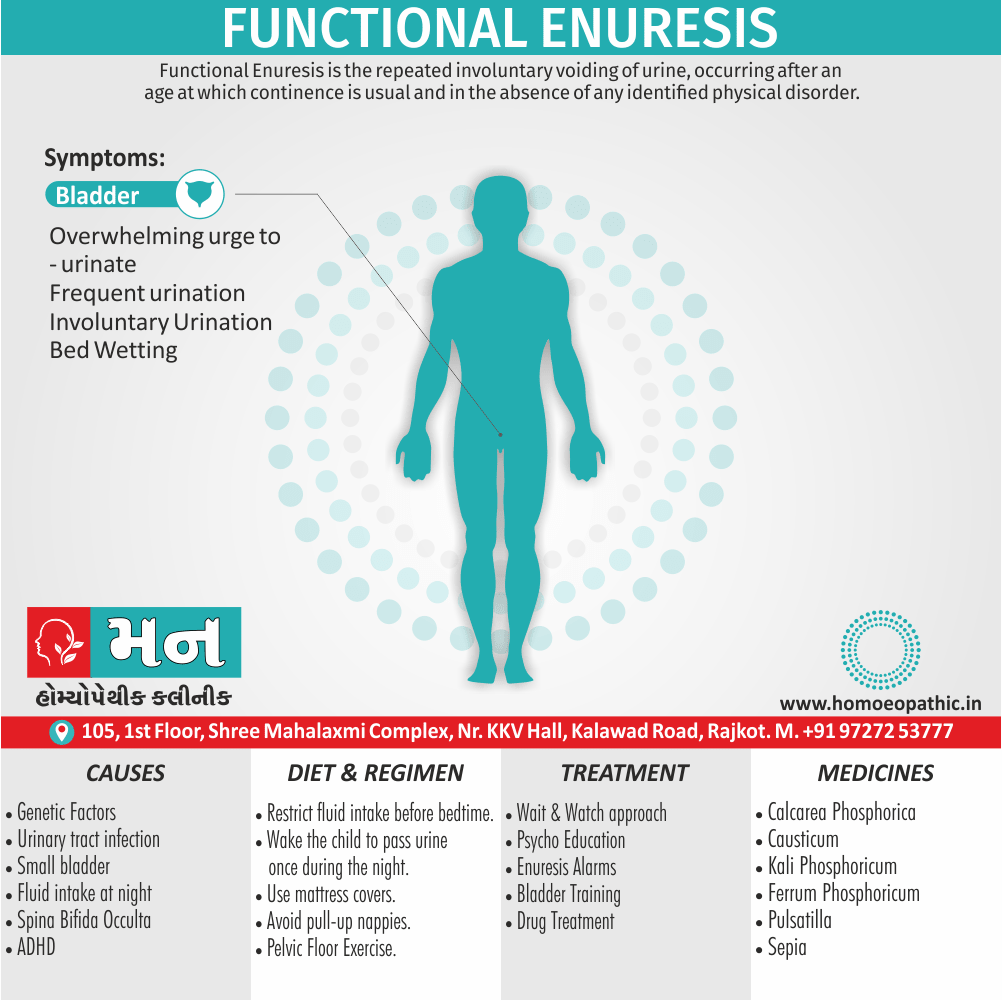
Functional Enuresis is the repeated involuntary voiding of urine, occurring after an age at which continence is usual and in the absence of any identified physical disorder. [1]
Overview
Epidemiology xxx
Causes
Types xxx
Risk Factors xxx
Pathogenesis xxx
Pathophysiology
Clinical Features xxx
Sign & Symptoms
Clinical Examination xxx
Diagnosis xxx
Differential Diagnosis xxx
Complications xxx
Investigations xxx
Treatment
Prevention xxx
Homeopathic Treatment
Diet & Regimen xxx
Do’s and Dont’s xxx
Terminology xxx
References
FAQ
Also Search As xxx
Overview
The condition may be nocturnal (bed-wetting), diurnal (occurring during waking hours), or both.
Nocturnal enuresis is referred to as primary if there has been no preceding period of urinary continence, and secondary if there has been a preceding period of urinary continence.
There is no absolute period of continence needed to become secondary enuresis, but 6 months is a commonly used time frame.
Most children achieve regular daytime and night-time continence by 3 or 4 years of age, and 5 years is generally taken as the youngest age for the diagnosis.
Nocturnal enuresis can cause great unhappiness and distress, particularly if the parents blame or punish the child, and if the condition restricts staying with friends or going on holiday.
Nocturnal enuresis occurs in about;
- 10 % of children at 5 years of age,
- 4 % at 8 years,
- 1 % at 14 years,
- 0.5 % in adulthood.
The condition is more frequent in boys. [1]
Daytime enuresis has a lower prevalence and is more frequent in girls.
Epidemiology xxx
Indian epidemiology then other
Causes
The majority of cases of nocturnal primary enuresis are idiopathic; there is simply a delay in maturation of the nervous system controlling the bladder.
These children often have a family history of enuresis, as children who have either one or two parents who were enuretic have a 44 and 70 % chance, respectively, of being enuretic themselves.
There are a range of other causes of enuresis, but these are more commonly associated with secondary nocturnal or diurnal enuresis.
Common causes of nocturnal primary enuresis:
- Idiopathic developmental delay
- Genetics
Less common causes of enuresis (consider in secondary nocturnal or diurnal cases):
- Urinary tract infection
- Diabetes mellitus
- Abnormalities of the urinary tract (e.g. small bladder, vesicoureteric reflux)
- Structural abnormalities of the nervous system (e.g. spina bifida occulta)
- Chronic constipation
- Diuretics: e.g. caffeine, alcohol
- ADHD
- Learning disorders or syndromes of developmental delay
- Behavioural: being too engaged in play or ‘leaving it too late’
- Psychological: i.e. a response to bereavement, stress, abuse, or bullying
- Obstructive sleep apnoea
- Epilepsy [1]
Other Causes:
- Fluid intake at night.
- The bladder is irritated by the bowels.
- Inability to know if the bladder is filled.
- Urinary tract infection.
- Stress also anxiety.
- Hyperactivity in children.
- Lack of attention.
Types xxx
AAA
Risk Factors xxx
Risk factors are things that make you more likely to develop a disease in the first place.
Pathogenesis xxx
Pathogenesis refers to the development of a disease. It’s the story of how a disease gets started and progresses.
Pathophysiology
Pathophysiology, on the other hand, focuses on the functional changes that occur in the body due to the disease. It explains how the disease disrupts normal physiological processes and how this disruption leads to the signs and symptoms we see.
Imagine a car accident. Pathogenesis would be like understanding how the accident happened – what caused it, the sequence of events (e.g., one car ran a red light, then hit another car). Pathophysiology would be like understanding the damage caused by the accident – the bent fenders, deployed airbags, and any injuries to the passengers.
In simpler terms, pathogenesis is about the "why" of a disease, while pathophysiology is about the "how" of the disease’s effects.
Clinical Features xxx
Tab Content
Sign & Symptoms
Nocturnal enuresis usually presents with voiding of urine during sleep in a child in whom it is difficult to wake. It may be accompanied by bladder dysfunction during the day which is termed non monosymptomatic enuresis.
Day time enuresis also known as urinary incontinence may also be accompanied by bladder dysfunction.
The symptoms of bladder dysfunction include:
1. Urge incontinence:
In detail, The presence of an overwhelming urge to urinate, frequent urination, attempts to hold the urine and urinary tract infections.
2. Voiding postponement:
Delaying urination in certain situations such as school.
3. Stress incontinence:
Generally, Incontinence that occurs in situations when increased intra-abdominal pressure occurs such as coughing.
4. Giggling incontinence:
Basically, Incontinence that occurs when laughing.
Secondary incontinence usually occurs in the context of a new life event that is stressful such as abuse or parental divorce. [2]
Clinical Examination xxx
Tab Content
Diagnosis xxx
Tab Content
Differential Diagnosis xxx
Complications xxx
Complications are what happen after you have a disease. They are the negative consequences of the disease process.
Investigations xxx
Tab Content
Treatment
Assessment:
- The majority of children who are bedwetting at 5 years will outgrow it in the next 2 years.
- Therefore, a watching and waiting approach is often the best option in this period.
- Many clinicians do not start to treat enuresis until 7 years unless it is causing functional, psychological, or social impairment.
- Most cases of primary enuresis can treat successfully in general practice.
Psychoeducation:
- The parents and their child should reassure that enuresis is common and the child is not to blame.
- The parents should told that punishment and disapproval are inappropriate and ineffective, and that they should reward success (e.g. with star charts), and not focus attention on failure.
- Reinforcing positives helps to increase self-esteem and also is a powerful tool in changing behaviour.
Practical advice:
Parents can be advised to:
- Restrict fluid intake before bedtime;
- Wake the child to pass urine once during the night;
- Use mattress covers;
- Avoid pull-up nappies (these can prolong the problem).
Enuresis alarms:
- A sensor to detect urine attached to the child’s pyjama trousers and a miniature alarm carry in the pocket or on the wrist.
- The child turns off the alarm and rises to complete emptying the bladder while the bed remade if necessary.
- In the past, before the necessary sensors were available, the passage of urine detect by two metal plates separated by a cotton pad.
- When the pad became wet, the current flowed and an alarm bell rang.
- The term pad and bell method is still in use to describe this approach to treatment.
- About 70 % of children improve within a month of this treatment, but a third relapse within a year.
Medication:
- The synthetic antidiuretic hormone analogue desmopressin (in other words, DDAVP) acts to reduce urine production whilst the child is asleep, and is effective at producing dry nights in 50 percent of children.
- It is available as an oral tablet or as a nasal spray, which is preferred by most children.
- Unfortunately, desmopressin has only a short-term effect and most children relapse as soon as they stop taking it.
- However, it can a useful method of allowing a child to attend a sleepover or camp.
- Tricyclic antidepressants, especially imipramine, are effective at reducing bedwetting when given at a low dose.
- Most children improve partially on the drug, and about a third stop completely, although most relapse when the drug stop.
- Because of this high relapse rate, the side effects of tricyclics, and the potential danger of accidental overdose, the use of antidepressant drugs limit mainly to enabling the child to dry over a short but important period, such as a school journey.
- It has a very limited longer-term role in those with persistent enuresis whose social, educational, or psychological development is being adversely affected by it.
Bladder training and pelvic floor exercises. [1]
Prevention xxx
Tab Content
Homeopathic Treatment
The remedies contained in this preparation bring about an improvement in nervous and debilitated constitutions. They also have an affinity to the motor nerves controlling the bladder functions.
Calcarea phosphorica: Constitutionally indicated in the asthenic patient.
Pulsatilla: Incontinence of urine, particularly in girls.
Ferrum phosphoricum: Incontinence of urine, also during the day.
Kali phosphoricum: Nervous constitutions. General debility and weakness.
Sepia: Specific affinity to the bladder sphincter (insufficiency of). Nocturnal enuresis during first sleep. Close relationship to sexual sphere.
Diet & Regimen xxx
Do’s and Dont’s xxx
Tab Content
Terminology xxx
Tab Content
References
- Psychiatry, Fourth Edition – Oxford Medical Publications -SRG-by John Geddes, Jonathan Price, Rebecca McKnight / Ch 32.
- https://en.wikipedia.org/wiki/Enuresis
FAQ
Frequently Asked Questions
What is Functional Enuresis?
Functional Enuresis is the repeated involuntary voiding of urine, occurring after an age at which continence is usual and in the absence of any identified physical disorder.
Homeopathic Medicines used by Homeopathic Doctors in treatment of Functional Enuresis?
- Calcarea phos
- Pulsatilla
- Ferrum phos
- Kali phos
- Sepia
What causes Functional Enuresis?
- Idiopathic developmental delay
- Genetics
- Urinary tract infection
- Diabetes mellitus
- Abnormalities of the urinary tract
- Structural abnormalities of the nervous system
- Chronic constipation
- Diuretics: e.g. caffeine, alcohol
- ADHD
What are the symptoms of Functional Enuresis?
- Urge incontinence
- Voiding postponement
- Stress incontinence
- Giggling incontinence
Also Search As xxx
Frequently Asked Questions (FAQ)
XYZ
XXX
XYZ
XXX
XYZ
XXX