Definition:
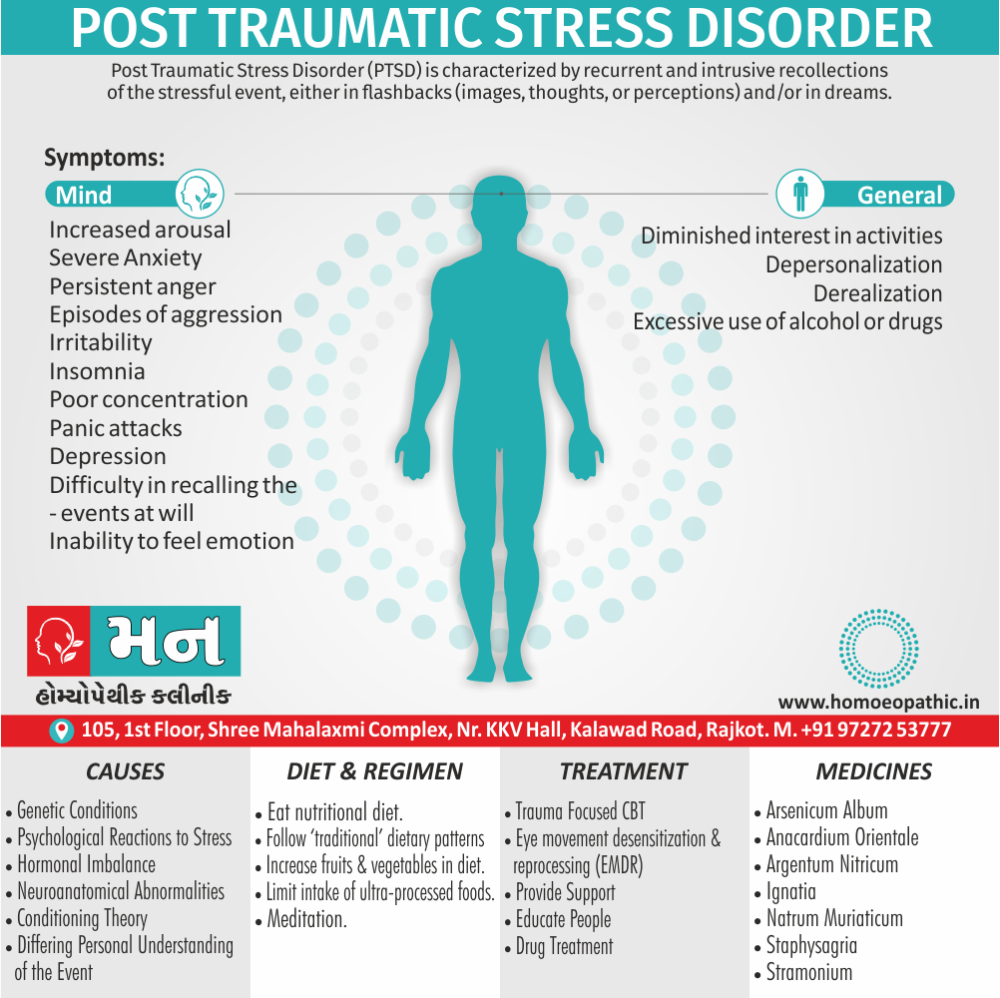
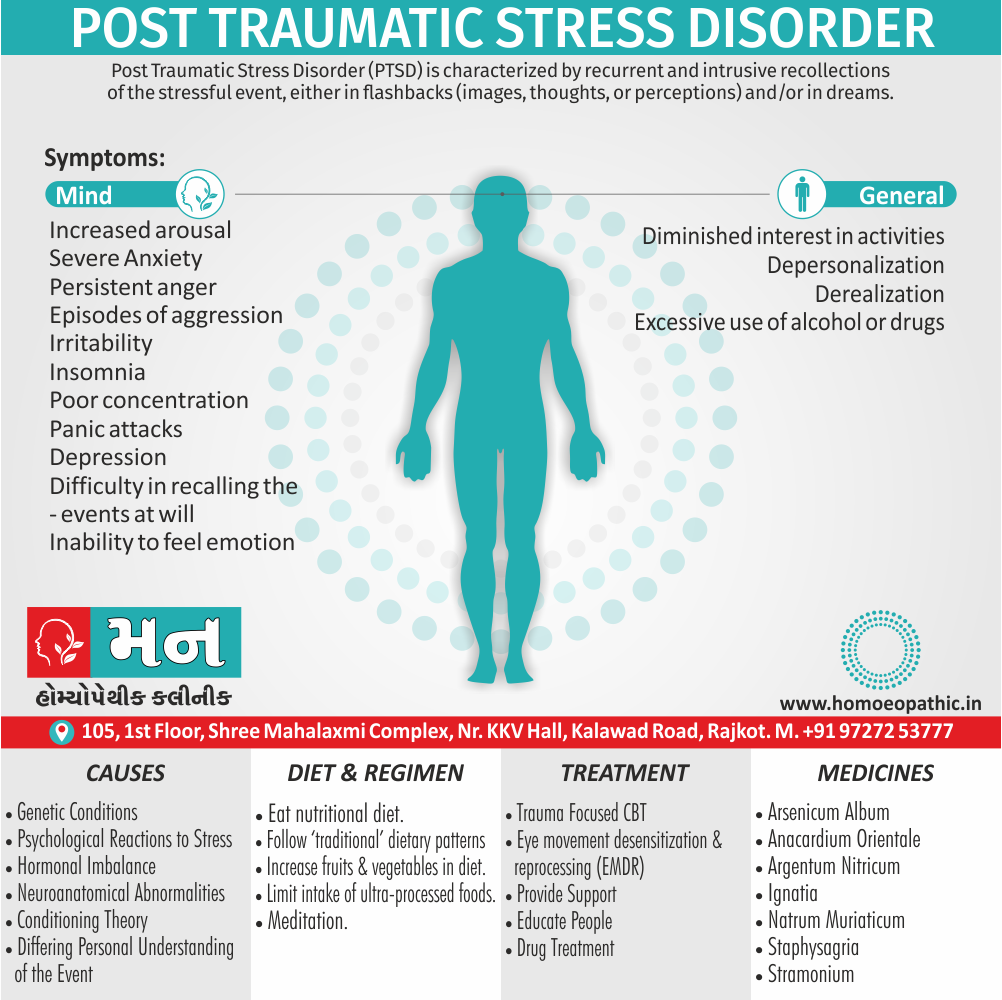
Post Traumatic Stress Disorder (PTSD) is characterised by recurrent and intrusive recollections of the stressful event, either in flashbacks (images, thoughts, or perceptions) and/or in dreams. [2]
Overview
Epidemiology
Causes
Types xxx
Risk Factors xxx
Pathogenesis xxx
Pathophysiology
Clinical Features xxx
Sign & Symptoms
Clinical Examination xxx
Diagnosis xxx
Differential Diagnosis xxx
Complications xxx
Investigations xxx
Treatment
Prevention xxx
Homeopathic Treatment
Diet & Regimen xxx
Do’s and Dont’s xxx
Terminology xxx
References
FAQ
Also Search As xxx
Overview
According to ICD-10, this disorder arises as a delayed and/protracted response to an exceptionally stressful or catastrophic life event or situation, which is likely to cause pervasive distress in ‘almost any person’ (e.g. disasters, war, rape or torture, serious accident).
The symptoms of Post Traumatic Stress Disorder (PTSD) may develop, after a period of latency, within six months after the stress or may be delayed beyond this period.
There is an associated sense of re-experiencing of the stressful event. There is mark avoidance of the events or situations that arouse recollections of the stressful event, along with marked symptoms of anxiety and increased arousal. [2]
A variety of terms have used to describe what we now call PTSD, including railway spine, stress syndrome, shell shock, battle fatigue, and traumatic war neurosis.
It is now recognized that PTSD is a relatively common disorder, with US citizens having a lifetime risk of developing the condition of 8 percent.
Effective treatments are available for PTSD, so it is an important condition to screen high-risk patients for, especially those who are being treated for physical injuries/diseases relating to the trauma. [1]
Epidemiology
Indian epidemiology then other
The US National Comorbidity Study found that 50 to 60 percent of individuals experience at least one traumatic event (fitting DSM-IV criteria) in their lifetime.
The most commonly experienced traumatic events are sudden death of a loved one, witnessing someone being killed or severely injured, accidents, and being involved in a fire.
However, most of those affected by traumatic events do not develop PTSD.
After a traumatic event of any type, the risk of developing PTSD is 8 percent for men and 20 percent for women.
The prevalence and incidence of PTSD vary markedly depending upon the geographical area studied.
Socioeconomic conditions, natural disasters, wars, and violence are not equally distributed across the world, and most of the current epidemiological figures relate to economically more developed countries.
In the USA, 7.8 percent of the population will suffer PTSD at some point in their lives, but the risk is twice as great for women (10 percent) as for men (5 percent). [1]
Causes
This refers to the initiating factors that trigger a disease process.
- Examples of causes include:
- Pathogens: Viruses, bacteria, fungi, parasites (infectious diseases)
- Genetic mutations: Inherited or spontaneous changes in genes (genetic diseases)
- Environmental factors: Toxins, radiation, nutritional deficiencies
- Lifestyle choices: Smoking, unhealthy diet, lack of exercise (contributing factors)
The necessary cause of post-traumatic stress disorder is an exceptionally stressful event in which the person was involved directly or as a witness.
Post Traumatic Stress Disorder (PTSD) is more common among those involved most directly in the stressful events, but the variation in response is not accounted for solely by the degree of personal involvement.
Predisposing factors:
1. Genetics i.e.:
Twin studies have shown a higher concordance of PTSD amongst monozygotic than dizygotic twins.
2. Physiological reactions to stress i.e.:
Patients with PTSD appear to have greater physiological reactions to stressors than people without PTSD who experienced the same traumatic event.
When stressed, patients show enhanced secretion of epinephrine and corticotropin secreting hormone, although levels of cortisol are lower than usual.
It seems that whilst the HPA axis is strongly stimulated, some abnormality occurs which enhances negative feedback. This may be an adaptation to reset the system in order to be able to respond quickly and strongly to new stressors.
Neurotransmitters also seem to be deregulated; the adrenergic activity of the sympathetic nervous system is increased, whilst levels and activity of serotonin (5HT) are decreased.
The fact that yohimbine (an alpha-receptor antagonist) provokes flashbacks whilst SSRIs decrease symptoms gives weight to this theory.
3. Neuroanatomical abnormalities i.e.:
MRI studies have shown that adults with PTSD have a smaller hippocampus than the general population.
Functional MRI has demonstrated that people with PTSD tend to show a heightened response to stress in the amygdala, hippocampus, and medial prefrontal cortex.
Maintaining factors:
1. Conditioning theory i.e.:
- This theory suggests that the continued symptoms of PTSD are due to classical conditioning.
- When a traumatic event occurs (an unconditioned stimulus), people respond with fear (unconditioned response).
- As reminders of the trauma occur (conditioned stimulus), people then respond with fear reactions (conditioned response).
- Frequently, the variety of stimuli widens, thereby increasing the symptom load.
- Avoidance of stimuli reinforces the conditioning, as it leads to reduced discomfort in the absence of a stimulus.
2. Differing personal understanding of the event i.e.:
- People have widely different views as to why the same event occurred, or what the future holds because of it.
- Some individuals will shake off a traumatic experience as a one of terrible event and move on. They tend to recover quickly.
- Patients with PTSD tend to have much more negative cognitions, often generalizing beyond the original event.
- Common examples are that the person starts to believe they were responsible for the accident that happened, or that nowhere is safe after being sexually assaulted.
- These negative cognitions reinforce themselves, similarly to those in patients with depression.
3. Stimuli triggering memories of the event i.e.:
- In a similar vein to the above, those patients who repeatedly come into contact with memories of the traumatic event tend to have symptoms for longer than those who do not.
- A good example of this is someone whose route to work passes the spot where a terrible car accident occurred.
4. Behaviours that maintain symptoms i.e.:
- Avoidance tends to stop people integrating the facts of the stressful experience into their memory, so that they continue to be fearful of the symptoms and what happened.
- Safety behaviours (e.g. constantly checking the gas hob is off after a fire) prevent a return to normality, and cause an increase in PTSD symptoms.
- Maladaptive coping strategies tend to increase the feelings of numbness and separation from the event, and do not help the person to acknowledge what has happened and continue with their life. [1]
Types xxx
AAA
Risk Factors xxx
Risk factors are things that make you more likely to develop a disease in the first place.
Biological:
- Females
- Age: Children and Older adults are particularly vulnerable
- Ethnic marginalized groups
- Family or personal psychiatric disorder
- Low intelligence
Psychological:
- Childhood abuse
- Low self-esteem
- Exposure to previous trauma
Social:
- Lack of social support
- Difficult economic or legal circumstances [1]
Pathogenesis xxx
Pathogenesis refers to the development of a disease. It’s the story of how a disease gets started and progresses.
This is the entire journey of a disease, encompassing the cause but going beyond it.
Pathophysiology
Pathophysiology, on the other hand, focuses on the functional changes that occur in the body due to the disease. It explains how the disease disrupts normal physiological processes and how this disruption leads to the signs and symptoms we see.
Imagine a car accident. Pathogenesis would be like understanding how the accident happened – what caused it, the sequence of events (e.g., one car ran a red light, then hit another car). Pathophysiology would be like understanding the damage caused by the accident – the bent fenders, deployed airbags, and any injuries to the passengers.
In simpler terms, pathogenesis is about the "why" of a disease, while pathophysiology is about the "how" of the disease’s effects.
Clinical Features xxx
Tab Content
Sign & Symptoms
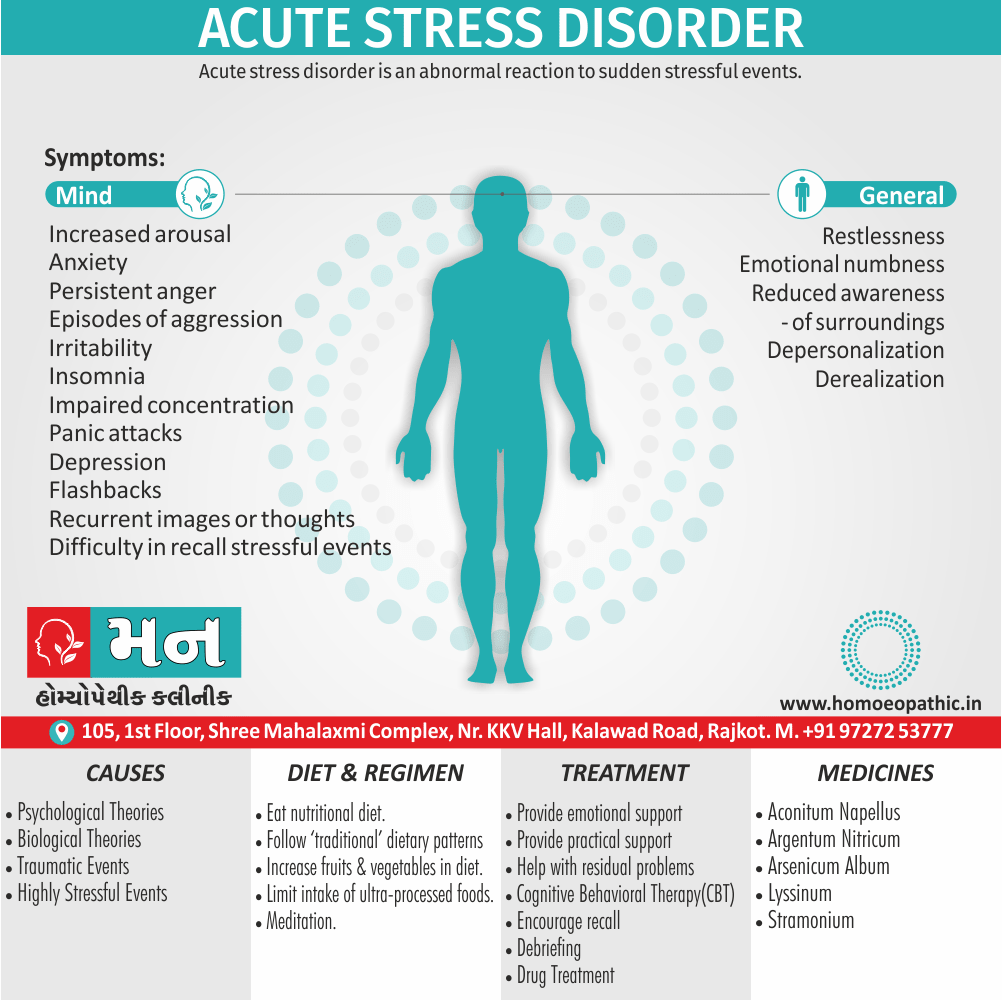
1. Increased arousal:
- Such as severe anxiety, irritability, insomnia, and poor concentration.
- There may be panic attacks and, occasionally, episodes of aggression.
- Anxiety increases further during flashbacks or reminders of the traumatic event.
2. Avoidance & ‘Dissociative’ symptoms:
- Such as difficulty in recalling the events at will, detachment, an inability to feel emotion (‘numbness’), and a diminished interest in activities.
- There is avoidance of reminders of the events and sometimes there is depersonalization and derealization.
3. Intrusions:
In this memories of the traumatic events appear suddenly as repeated intense imagery (‘flashbacks’), vivid memories, intrusive repetitive thoughts, or distressing dreams.
4. Depressive symptoms:
They are common, and survivors of a major disaster often feel guilt.
5. Maladaptive coping responses:
This include persistent anger (especially among those who believe they are innocent victims of others’ misbehaviour), excessive use of alcohol or drugs, and episodes of deliberate self-harm, some of which end in suicide.
Avoidance of reminders of the stressful events.
Maladaptive coping strategies. [1]
Post-traumatic stress disorder is diagnosed when symptoms last for 4 weeks or longer.
Clinical Examination xxx
Tab Content
Diagnosis xxx
Tab Content
Differential Diagnosis xxx
Complications xxx
Complications are what happen after you have a disease. They are the negative consequences of the disease process.
Investigations xxx
Tab Content
Treatment
Assessment:
A full psychiatric history should be taken, including information from the patient, a third-party informant, primary care physician, and previous hospital notes.
Specific points to cover include:
- The nature and severity of the stressful event;
- Current symptoms, including duration and severity;
- Effect of symptoms upon life at home, work, school, etc.;
- The patient’s beliefs about the nature of their condition;
- Previous diagnoses of psychiatric conditions and treatments received for them;
- Family history of psychiatric conditions;
- Current medications (prescribed, illicit, over-the-counter, alcohol, caffeine, nicotine);
- Premorbid personality traits;
- Current social situation: accommodation, employment, finances.
General measures:
- Provide support (practical, emotional, social, self-help materials)
- Information and education about PTSD
- Help with associated guilt, grief, or anger
Encourage talking about the event to friends and family, and finding ways to understand what has happened.
This helps to integrate memories of the event with the rest of the person’s experience and to find a way for them to continue with their life.
Psychological treatments:
Watchful waiting (symptoms for less than 4 weeks).
For patients presenting with symptoms that are severe or have persisted for 3 months after the trauma, psychological therapy should be offered.
Occasionally, patients may have severe disabling symptoms soon after the event, and they should be offered psychological therapy too.
There are two main types of therapy that are effective at reducing the symptoms of Post Traumatic Stress Disorder (PTSD):
1. Trauma-focused CBT i.e.:
- CBT is the first-line choice, and should be offered to all patients with PTSD.
- Specialized CBT for PTSD includes both exposure and cognitive therapy.
- The exposure element involves helping the patient to remember and put together memories of the events, and to relive the stressor with an emphasis on discussing their thoughts and feelings during the process.
- In vivo exposure is also used, in which the patient gradually works up to confronting situations they had avoided because they reminded them of the trauma.
- Common examples include visiting the site of an attack, or driving again after an accident.
It is thought that exposure works in two ways i.e.:
- Getting the patient used to being in the situation again (habituation),
- Organizing their memories such that they can identify that intrusive re-experiences are recollections, and are not happening right now.
The therapist helps the person to challenge these beliefs and to change their behaviours surrounding them.
A completed course of CBT reduces symptoms to a clinically insignificant level in 60 percent of patients.
2. Eye movement desensitization and reprocessing (EMDR) i.e.:
- This is another specialize treatment that assists the patient to process memories of the traumatic event and feel more positive about it.
- The patient has told to track the therapist’s finger as they move it rapidly back and forth in front of them, which induces sadistic eye movements.
- During this process the patient is suppose to focus on a trauma-related image, and then afterwards to discuss the thoughts and emotions that surround it.
- This is repeat many times while focusing on different images.
Pharmacological therapies:
Drugs should not use as the first-line treatment, but should reserve for those patients who are unable to undertake therapy, fail to improve with therapy, or have comorbid depression.
Hypnotics i.e.:
- A short-term course of a hypnotic can give for insomnia, especially in the immediate aftermath of a traumatic event.
- A maximum of 3 weeks should prescribe due to the risks of tolerance and dependence.
- A good choice is a short-acting benzodiazepine (e.g. temazepam).
Antidepressants i.e.:
- Approximately 60 percent of patients will respond to an SSRI, although more than one may need to try to eliminate symptoms altogether.
- The first-line choice in the UK should an SSRI, and paroxetine has the greatest evidence base.
- Mirtazapine and amitriptyline can try if an SSRI is not successful, but they should initiate by a psychiatrist.
- The drug should continue for at least 12 months after symptoms resolve, then tapered slowly.
- If a patient does not respond to medication, check their compliance, increase the dose of the drug, or try another class.
- Occasionally, patients will need to add an atypical antipsychotic (e.g. olanzapine) to their antidepressant. [1]
Prevention xxx
Tab Content
Homeopathic Treatment
Recommended medicines for Post Traumatic Stress Disorder (PTSD) are Natrum Muriaticum, Ignatia, and Kali Phosphoricum.
Natrum Muriaticum acts well for PTSD when a person tends to dwell on past unpleasant memories. The person wants to isolate and is afraid of new relationships.
Ignatia, an excellent medicine for PTSD, is of great help when frustration and hopelessness accompany PTSD. Ignatia also works well when a person is quarrelsome and has many changes in mood.
Kali Phosphoricum is a well-indicated medicine for PTSD when night terrors accompany it. In such cases, patients have an aversion to meeting people and talking to them.
1. For PTSD with Flashbacks of Past Unpleasant Events:
Staphysagria and Nitric Acidum are considered as top-grade medicines in the treatment for PTSD when flashbacks of previous unpleasant events occur.
- Staphysagria acts well when a person keeps dwelling on past unpleasant incidents of rape or sexual abuse. The patient tends to throw or break things.
- Nitricum Acidum is a very effective medicine for PTSD in cases where a person holds grudges also dwells on past horrifying incidents. In detail, Nitricum Acidum treats symptoms like violent anger and hatred for the people who have offended.
2. For PTSD Accompanied by Disturbed Sleep:
The most effective remedies for PTSD accompanied by disturbed sleep are Opium and Coffea.
- Opium acts well in cases of PTSD when a person is sleepy but is unable to sleep. The person develops a fear after the fright, which remains for a long time.
- Coffea works well in cases where there is sleeplessness with a continuous flow of ideas in the mind. Mental activity keeps a person awake and makes him restless.
3. For PTSD with Nightmares:
Excellent remedies for PTSD accompanied by nightmares are Arsenic Album and Staphysagria.
- Arsenic Album is a beneficial medicine for PTSD in cases where there are nightmares and restlessness. In such situations, the patient has dreams of dead persons, fire, and darkness.
- Staphysagria, a well-selected medicine for PTSD, works well, especially in children. Usually, the child screams, wants everybody to go out and calls for the mother.
4. For PTSD with Delusions or Hallucinations:
Prominent remedies for PTSD along with delusions or hallucinations are Agaricus Muscarius and Hyoscyamus.
- Agaricus Muscarius is a well-indicated treatment for PTSD when the person is preoccupied with thoughts of death, graves, and dying.
- Hyoscyamus, another effective remedy, acts well when a person talks to imaginary characters and also imagines he is in the wrong place.
5. For PTSD with Indifference:
Top remedies specifically for PTSD accompanied by indifference are Sepia and Aurum Metallicum.
Sepia is very useful in persons who show an aversion to family, friends, company, also sympathy.
Aurum Metallicum acts well while dealing with patients who have lost love. In such cases, patients tend to died by suicide, and imagine they are unfit for the world.
6. For PTSD when a Person Wants Solitude:
Natrum Muriaticum and Ignatia are excellent remedies for PTSD when a person wants to be alone.
Homeopathy can be of great help in depression.
Natrum Muriaticum is of great help in cases of severe depression and feelings of isolation. In such situations, the person shuts down emotionally also closes off from others after the traumatic event.
Ignatia is a well-chosen remedy especially for patients who want to be alone and cannot tolerate contradiction. Additionally, Other symptoms include indifference, excessive emotion, moodiness, and an aversion to any amusement.
7. For PTSD with Anger:
Top grade remedies for PTSD accompanied by anger are Chamomilla also Nux Vomica.
Chamomilla works well in cases where the patient gets involved in disputes and quarrels without a valid reason. In detail, The patient also tends to dwell on past disagreeable occurrences and keeps on moaning.
Nux Vomica is a very effective medicine for PTSD when the patient is impatient when spoken to, spiteful, violent also angry without provocation.
8. For PTSD with Difficulty in Concentration:
Basically, Anacardium and Kali Phosphoricum are excellent remedies for PTSD for patients experiencing difficulty in concentration and memory. [3]
Diet & Regimen xxx
Do’s and Dont’s xxx
Tab Content
Terminology xxx
Tab Content
References
- Psychiatry, Fourth Edition – Oxford Medical Publications -SRG-by John Geddes, Jonathan Price, Rebecca McKnight / Ch 23.
- A Short Textbook of Psychiatry 7th edition by Niraj Ahuja / Ch 8.
- https://www.drhomeo.com/homeopathic-treatment/homeopathic-treatment-ptsd/
FAQ
Frequently Asked Questions
What is Post Traumatic Stress Disorder?
Post Traumatic Stress Disorder (PTSD) is characterised by recurrent and intrusive recollections of the stressful event, either in flashbacks (images, thoughts, or perceptions) and/or in dreams.
Homeopathic Medicines used by Homeopathic Doctors in treatment of Post Traumatic Stress Disorder?
- Natrum Muriaticum
- Ignatia
- Kali Phosphoricum
- Staphysagria
- Nitricum Acidum
- Opium
- Coffea
What causes Post Traumatic Stress Disorder?
- Genetics
- Physiological reactions to stress
- Neuroanatomical abnormalities
What are the 5 symptoms of Post Traumatic Stress Disorder?
- Increased arousal
- Avoidance & ‘Dissociative’ symptoms
- Intrusions
- Depressive symptoms
- Maladaptive coping responses
Also Search As xxx
Frequently Asked Questions (FAQ)
XYZ
XXX
XYZ
XXX
XYZ
XXX
How can I find reputable homeopathy clinics or homeopathic doctors in my area?
You can found Homeopathic Clinic For XXXX by searching for
Specific city Examples are
You can also search for near you Examples are